
This could inform new ways of working and commissioning decisions to improve care for people living with frailty who are at risk of falls and fracture. Public Health Birmingham is working with GP practices across the 3 CCGs in Birmingham using eFI to understand current frailty provision and identify any gaps. Routine frailty identification can help local clinicians and commissioners to review current service provision. There are a series of webinar recordings available to support the implementation of routine frailty identification into primary care. Age UK, NHS and Public Health England leaflet on frailty for patients called Keeping your independence.Yorkshire and Humber Academic Health and Science Network on Recognising and managing frailty.Walk a short distance (approximately 3 meters). Sit comfortably in a straight-backed chair. NHS England Toolkit for general practice on supporting older people living with frailty Get Up and Go Test (GUG) GUG Instructions: Ask the patient to perform the following series of maneuvers: 1.NHS England guidance for general practices on Supporting routine frailty identification and frailty through the GP Contract 2017/2018.NHS Digital publish relevant local, regional and national data on frailty.To support routine frailty identification in primary care there are a number of resources: The eFI is a risk stratification tool and not intended to be used as a diagnostic tool.Ĭonfirmation of frailty in an individual should be undertaken using a validated tool such as: Early identification coupled with targeted support can help older people living with frailty to stay well and live independently for as long as possible. It targets a small number of key interventions (falls assessment, medicines review and promotion of the additional information in the summary care record) at those most at risk of adverse events including hospitalisation, nursing home admission and death. The eFI uses routine health record data to automatically calculate a score which can identify whether a person in likely to be fit or living with mild, moderate or severe frailty.Ĭhanges to the GP contract in 2017/18 introduced routine frailty identification for patients who are 65 and over. This can be done using the electronic Frailty Index (eFI) or any other appropriate assessment tool. The NHS in England is the first health system in the world to systematically identify people, aged 65 and over, who are living with moderate and severe frailty using a population-based stratification approach. Ageing well and supporting people living with frailty.Living well, ageing well and tackling premature mortality.To actually understand how treatments ameliorate patients' mobility, ITUG with TUG task duration measurement should be preferred to TTD.īalance and locomotor impairment Elderly ITUG Instrumental timed up and go test Rehabilitation Responsiveness.Ĭopyright © 2019 Elsevier B.V. 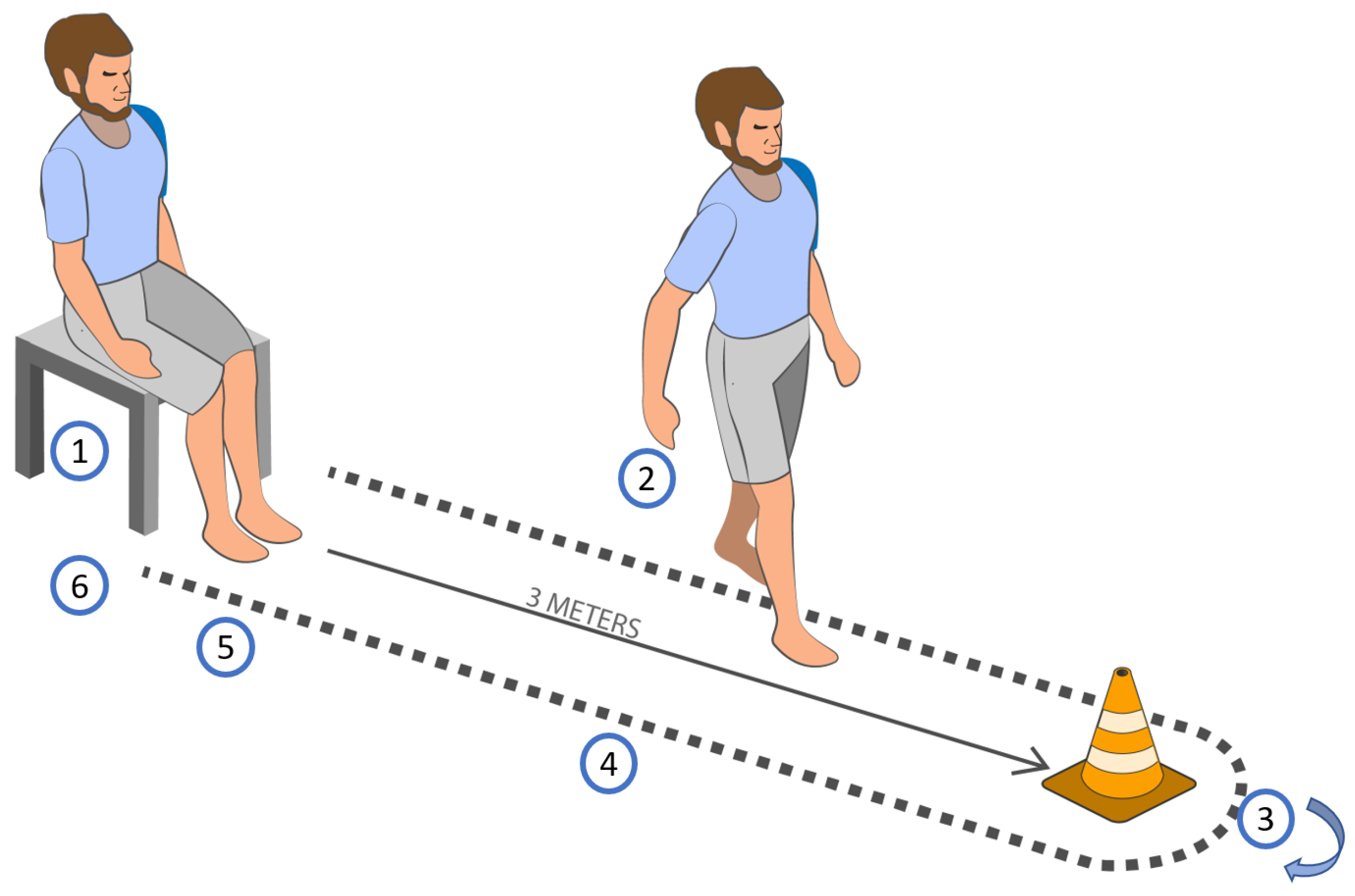
Moreover, when TTD has improved there is at least a TUG task that has improved, but that remains unknown. In most cases, TTD improvement is not associated with the improvement of all TUG tasks. The improvement of all TUG tasks can be only inferred in the (unusual) event of a large TTD shortening (AP: >39%, LR + AP = 6.26 CP: >30%, LR + CP = 9.0). If TTD has improved, there is at least one TUG task that actually improved (LR + AP = 3.17 LR + CP = 9.54). Conversely, if TTD has not improved, not even a single TUG task has improved (LR - AP = 0.13 LR - CP = 0.19). TTD improvement per se is not enough to claim that all the TUG tasks have improved (LR + AP = 1.32 LR + CP = 1.85). TTD and TUG tasks have improved if at least four measurements on discharge were shorter than the shortest measurement on admission. Likelihood ratios (LRs) were used for inferring TUG tasks improvement from TTD improvement. TTD and TUG tasks duration was measured on admission and discharge (five trials/session) by means of the instrumental TUG test (ITUG). This retrospective study recruited 120 elderly patients (mean, SD: 76.9, 6.6 years) admitted to inpatient rehabilitation because of an acute or chronic neurological disease (acute patients, AP chronic patients, CP). walking and turning), the total TUG duration (TTD) is usually the only outcome measure, with TTD shortening indicating the patient's improvement.ĭoes TTD shortening reflect the improvement of each TUG tasks or does it reflect the improvement of only some of them? Although the TUG test consists of different tasks (e.g. The timed up and go (TUG) test is widely used for assessing treatments effectiveness on elderly mobility.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
